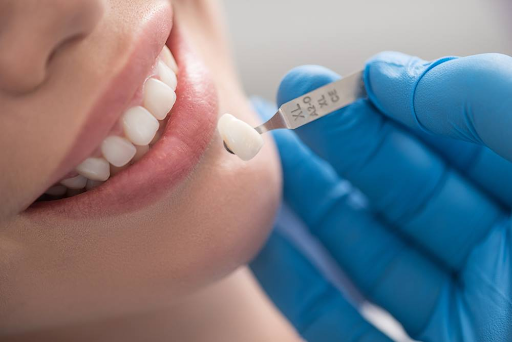
- Invest in Your Smile: The Value of Porcelain Veneers Cost
- Bridging the Digital Divide: Navigating the Affordable Connectivity Program
- A Culinary Tour of NYC: The 50 Best Restaurants You Must Try
- Navigating the Digital Jungle: How to Block Robocalls Spam Calls and Texts
- Rena Monrovia When You Transport Something by Car